To stave off Alzheimer’s, protect your brain’s mitochondria

- Known as the cell’s powerhouse, mitochondria are crucial for memory preservation and are emerging as key players in the fight against Alzheimer’s, with damaged mitochondria being linked to the disease’s progression.
- Despite significant investment, traditional research targeting beta-amyloid plaques and tau proteins has largely failed in human trials, leading to a shift in focus towards mitochondrial health as a potential root cause.
- Regular exercise and an antioxidant-rich diet are essential for supporting mitochondrial function, potentially offering protection against Alzheimer’s and other age-related conditions.
One of the few facts people seem to remember from middle school biology is that mitochondria are the powerhouses of the cell. In what is either delicious vindication or the worst of ironies, let us never forget that fact, since mitochondria also appear to play a role in preserving our memories. Indeed, they may be the key to the fight against Alzheimer’s disease.
An increasing body of research points to damaged or dysfunctional mitochondria as a driver of Alzheimer’s disease with healthy mitochondria being the ticket to staving off decline. This is fantastic news for the 10% to 20% of people who will be diagnosed in their lifetimes, because it provides a new target for researchers. Of course, the path to healthy mitochondria seems to be the same as the one for preventing cancer, heart disease, or a host of other age-related maladies: exercise and a diet rich in antioxidants. Yes, it’s the same boring advice, apparently because it works.
A story of failure
The story of Alzheimer’s research is one of failure. In the U.S. alone, 5.8 million people live with Alzheimer’s, and despite over 100 years and $3.7 billion spent to find a cure, there is none. For decades, the targets of research have been a buildup of protein fragments between neurons called beta-amyloid plaques and tangled proteins inside neurons called tau. Time and again, researchers would achieve success at reducing plaques and tangles in rodents only to find that the new treatment had little effect on humans.
In the words of drug chemist Derek Lowe in Science magazine’s In the Pipeline, “Every single one of these interventions has failed in the clinic. Every last damn one.” (Coincidentally, though he was cleared of any wrongdoing, Stanford University president Marc Tessier-Lavigne recently resigned after “serious flaws” were revealed in research that he published regarding Alzheimer’s.)
Even the new amyloid targeting drug Leqembi — the first in two decades to receive full FDA approval — falls far short. It comes with a risk of potentially fatal brain swelling and bleeding and only slows cognitive decline by five months over a period of 18 months in patients with mild dementia. Some experts say that the effects may not be enough for patients or family to notice.
Many scientists now suspect that plaques and tangles are not the cause, but merely a downstream symptom. What lies upstream is mitochondrial health.
Protect your brain’s mitochondria
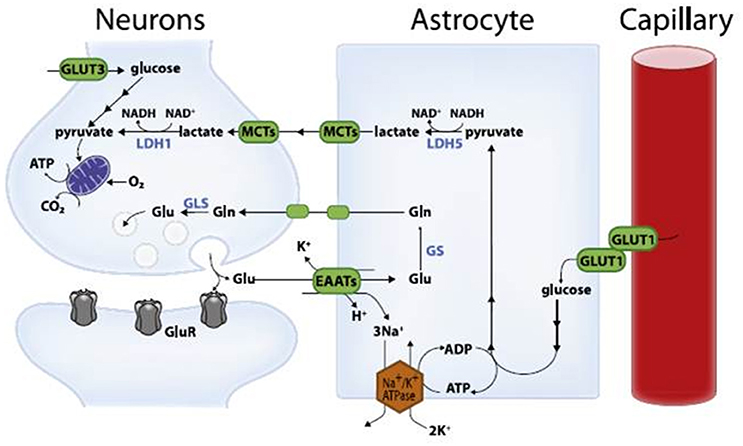
As you might suspect from the “powerhouse” analogy, mitochondria change food into energy. But they also store calcium, destroy cells that aren’t working properly, and generate heat. When mitochondria weaken, they produce less ATP (a molecule that can be thought of as “energy currency”), mismanage calcium ion concentrations, create an overabundance of damaging reactive oxygen species, and don’t regenerate effectively. And because our brains are low on antioxidants while running hot, sucking up a fifth of our total calories and oxygen, they are particularly sensitive to oxidative damage. In short, the brain needs mitochondria to stay in tip-top shape.
But they don’t. Mitochondrial dysfunction is linked to aging and Alzheimer’s disease, occurring even before clinical symptoms appear. Recent studies also suggest a link between abnormally functioning mitochondria and overabundant tau proteins.
Exercise is key to keeping your mitochondria healthy. Endurance training enhances mitochondrial activity and has been shown in mice to protect against brain atrophy. In studies with Alzheimer’s patients, exercise increased blood flow to the brain, thickened the hippocampus, enhanced growth of new neurons, and improved cognitive performance. Alternatively, a sedentary lifestyle increased damaging reactive oxygen species, increased inflammation in the brain, and reduced mitochondrial activity.
To measure mitochondrial fitness, the best metric is VO2 max, which represents the maximum rate that your body can use oxygen during exercise. Essentially, it reflects the body’s ability to utilize oxygen for energy production (and, remember, mitochondria are producing that energy). While a direct measure of your VO2 max requires special equipment, most fitness watches provide an indirect VO2 max estimate. In the Fitbit and Apple Watch this is called the “cardio fitness level.” Numbers vary for men and women, but for best results, aim high.
Aside from exercise, mitochondrial health improves with an antioxidant-rich diet full of plants, like blueberries, red beans, tomatoes, spinach, artichokes, and green tea. Studies show that calorie restriction and ketogenic diets may also be protective. And stay away from stress. In animal studies, chronic stress, anxiety, low social status, aggression, social defeat, and fear all damage mitochondria.
Of course, even a person who follows this advice can still get Alzheimer’s. But knowing that mitochondria appear to play a crucial role in its development will give scientists plenty to think about as they research new drugs to stave off this devastating disease.