New cancer ‘vaccine’ helps immune system find, kill disease

Pixabay
- In a recent clinical trial, three of 11 patients saw significant regression or complete remission of lymphoma.
- The approach is an immunotherapy, a relatively young field in cancer research that involves directing the immune system to kill cancer cells on its own.
- The researchers suggested their approach might improve the efficacy of existing immunotherapies.
Promising results from a recent medical trial suggest scientists might soon be able to redirect the immune system to destroy cancer.
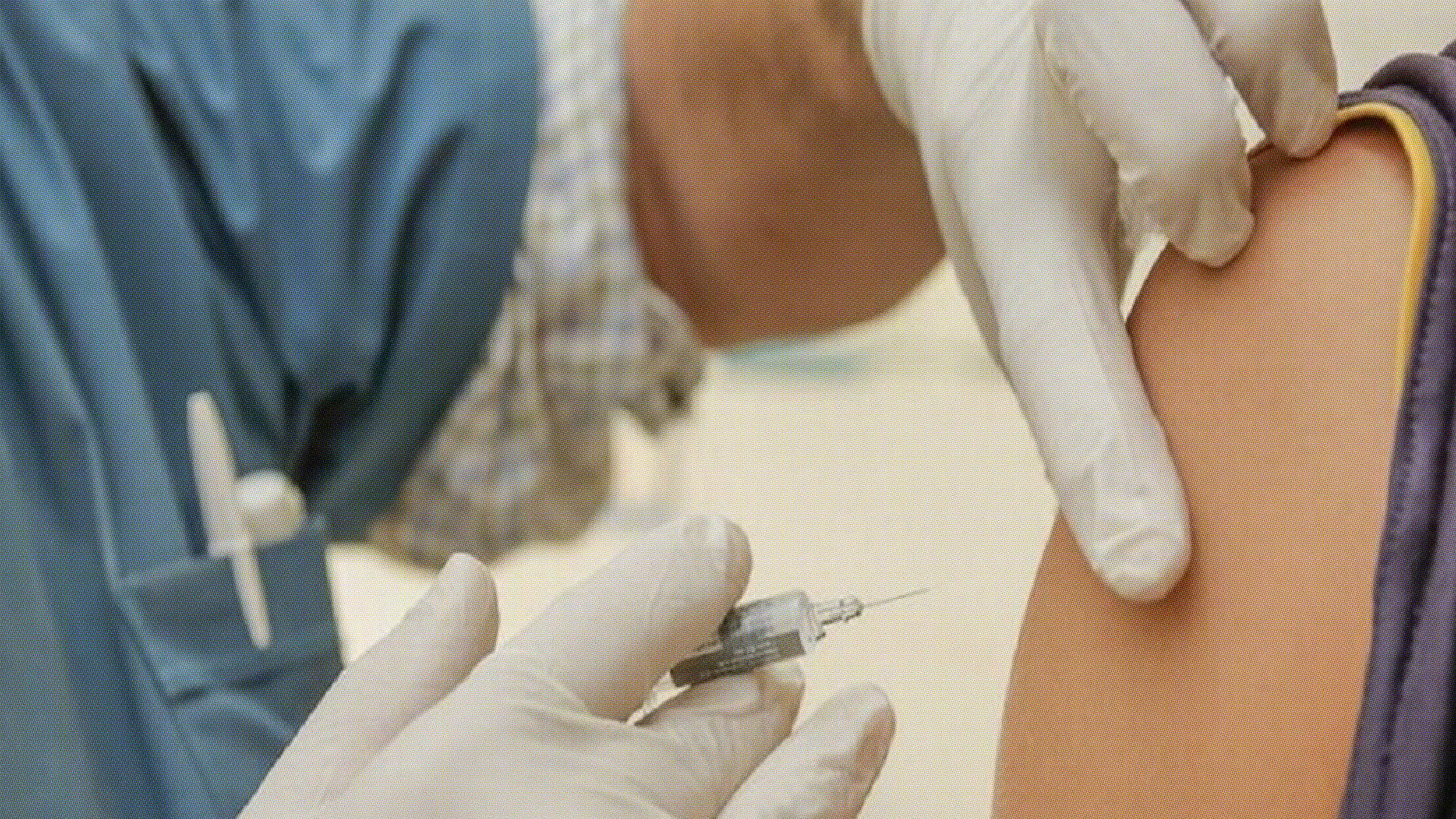
The immunotherapy approach — dubbed “in situ vaccination” by researchers at Mount Sinai — works somewhat similar to a vaccine. In the study, published in the journal Nature on April 8, 11 participants had one of their tumors injected with a steroid that recruits dendritic cells to the site. The participants then underwent a low dose of radiation, and were also given another stimulant to activate the dendritic cells, which then direct cancer-fighting T-cells to kill any tumors they encounter throughout the body.
“We’re injecting two immune stimulants right into one single tumor,” senior researcher Dr. Joshua Brody told HealthDay. “We inject one tumor and we see all of the other tumors just melt away.”
It’s too early to know exactly what to make of the results, however, and only three of the 11 patients saw their disease (non-Hodgkin’s lymphoma) go into significant regression or complete remission. Still, cancer was halted in six of the patients for three to 18 months.
“It’s really promising, and the fact you get not only responses in treated areas, but areas outside the field [of treatment with radiation] is really significant,” Dr. Silvia Formenti, chairwoman of radiation oncology at Weill Cornell Medicine and NewYork-Presbyterian, who wasn’t involved in the study, told CNBC.
Why immunotherapies are the focus of intense study
Immunotherapy is a relatively young field in cancer research. It’s gained traction in recent years because of its alluring promise: kill cancer not with harmful, dangerous drugs or radiation, but rather by harnessing the power of the body’s immune system.
In 2018, James Allison and Tasuku Honjo won the 2018 Nobel Prize in Physiology or Medicine for their innovative work in developing immunotherapy treatments and for bringing them closer to mainstream acceptance and study.
“Allison’s and Honjo’s discoveries have added a new pillar in cancer therapy. It represents a completely new principle, because unlike previous strategies, it is not based on targeting the cancer cells, but rather the brakes — the checkpoints — of the host immune system,” Klas Kärre, a member of the Nobel Committee and an immunologist at the Karolinska Institute in Stockholm, said in a statement. “The seminal discoveries by the two laureates constitutes a paradigmatic shift and a landmark in the fight against cancer.”
There are multiple types of immunotherapy. The one Kärre describes here is called checkpoint blockade, the approach that put former President Jimmy Carter’s melanoma in remission in 2015. This immunotherapy technique involves administering drugs that release the immune system’s “brakes” which, as the National Cancer Institute describes, “keep T cells (a type of white blood cell and part of the immune system) from killing cancer cells. These drugs do not target the tumor directly. Instead, they interfere with the ability of cancer cells to avoid immune system attack.”
The recent clinical trial was only conducted on patients with lymphoma, but the researchers suggested their approach could be potentially used to treat other types of cancer — and that it could improve the efficacy of other immunotherapies, including checkpoint blockade.
“The in situ vaccine approach has broad implications for multiple types of cancer,” said Brody, the study’s lead author and the director of the Lymphoma Immunotherapy Program at The Tisch Cancer Institute at the Icahn School of Medicine at Mount Sinai. “This method could also increase the success of other immunotherapies such as checkpoint blockade.”