New peanut allergy treatment could save kids’ lives, researchers say

Pixabay Commons
- The trial included hundreds of participants with peanut allergies.
- The oral regimen contained trace amounts of peanut protein, and participants would take increasing amounts of the protein over the course of six months, with the goal being to retrain the immune system.
- By the end, about two-thirds of participants were able to consume peanut protein without showing any allergic symptoms.
A new treatment could soon help reduce the severity of peanut allergy reactions in children, and also ease the anxieties that accompany the life-threatening condition.
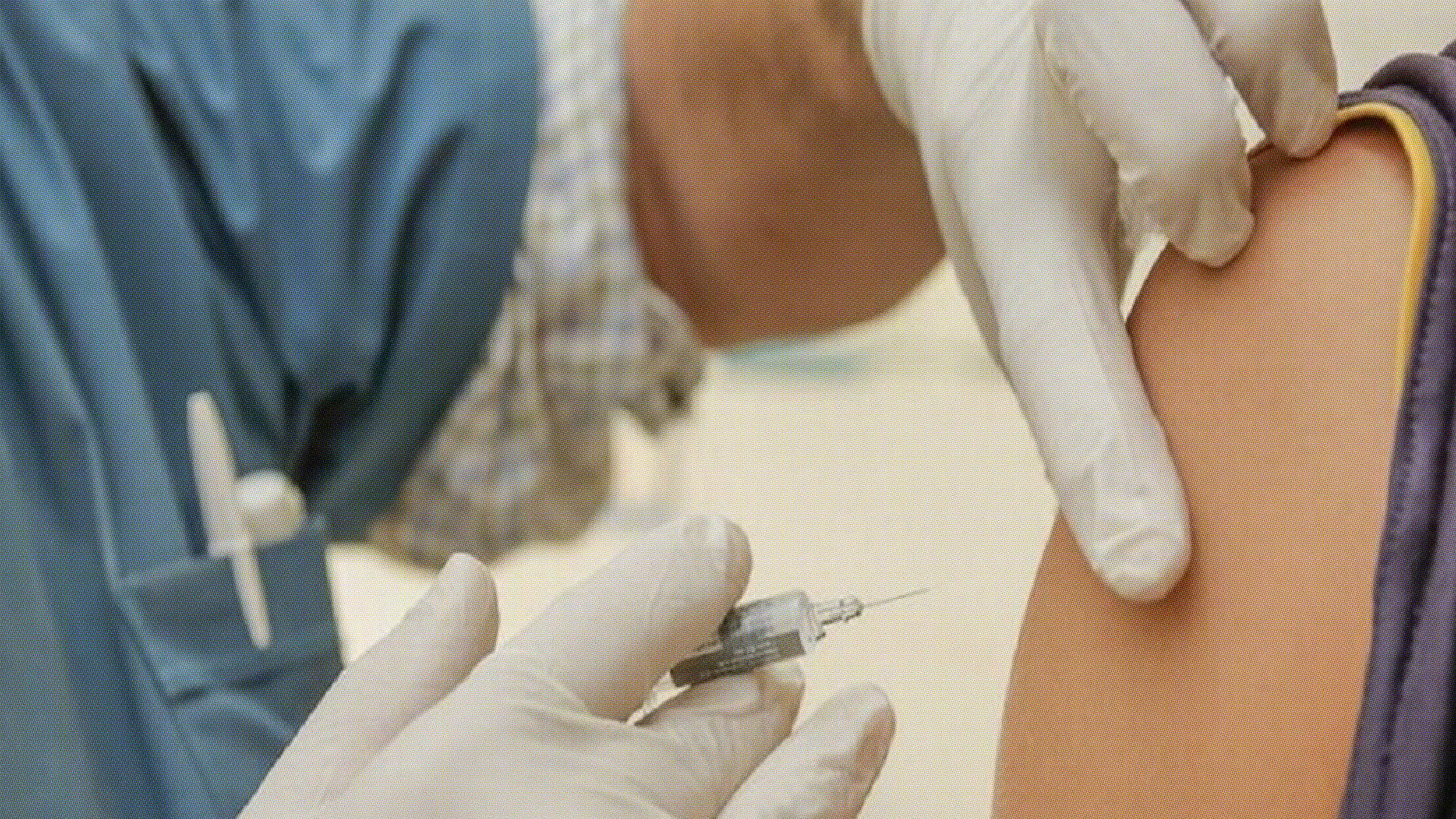
The treatment is an oral immunotherapy regimen that contains tiny amounts of peanuts. It’s designed to gradually expose children to the food and build tolerance to it over the course of six months under supervised medical care. The goal isn’t to eliminate the allergy but to reduce the severity of a reaction should one occur.
Recently, hundreds of children received the regimen while participating in a double-blinded, placebo-controlled trial that lasted six months. The results were largely promising: About two-thirds of the children were able to consume about 600 milligrams or more of peanut protein—the equivalent of two peanuts—without developing allergic symptoms, as the New York Timesreports.
“This trial is the most definitive look at whether this treatment is right for patients,” Dr. Brian P. Vickery, the lead author of a new paper on the trial, told the Times. “It has generated the highest quality evidence to date about whether oral immunotherapy works and how safe it is.”
Still, the results were mixed, as Vickery and his colleagues announced Sunday at a conference of the American College of Allergy, Asthma & Immunology in Seattle. Here’s a quick breakdown of the recent trial, which studied the effects of a “peanut-derived investigational biologic oral immunotherapy drug” called AR101 and developed by Aimmune Therapeutics.
- 551 people participated, 496 of whom were 4 to 17 years old. All participants had peanut allergies, and displayed allergic reactions after consuming as little as one-third of a peanut.
- The goal was to feed participants a daily dose of peanut protein, starting at just 3 milligrams and building incrementally to 300 milligrams over six months. That period would be followed by a six-month maintenance course, during which participants would take 300 milligrams everyday.
- Half of people who completed the trial could withstand taking 1,000 milligrams of peanut protein.
- However, almost all of the children showed some adverse side effects during the study.
- 4.3 percent of children who received the active drug showed severe side effects, compared to less than 1 percent of the children on placebo.
- 20 percent of children who received the active drug withdrew from the study, most of them due to negative side effects.
- 14 percent of people who received the active drug received injections of epinephrine. One child experienced anaphylaxis and required three EpiPen injections. Only 6.5 percent of people who took the placebo received epinephrine.
How immunotherapy work for allergies
Allergy shots, tablets and oral treatments, like the one used in the recent study, are all forms of allergen immunotherapy. The idea behind all approaches is to retrain the immune system by gradually exposing the body to a particular allergen. After a period of regular exposure, the body typically becomes more desensitized to the allergen, making allergic reactions less severe.
The idea for immunotherapy traces back to the early 20th century when scientists noted that people with hay fever sometimes lose their allergy because they “have had the good fortune to develop an active immunity against the toxin,” as pathologist Leonard Noon, who’s credited with discovering the benefits of immunotherapy, once wrote.
Hopefully, the new treatment will bring similar good fortune to the .6 to 1 percent of the population who suffer from peanut allergies.
“It’s pretty exciting,” Carolee Grodi, a mother of a child in the recent trial, told the Times. “It’s not eradication of the allergy, it’s just protection against an accidental exposure, but that’s huge. People don’t realize it, but peanuts are everywhere.”
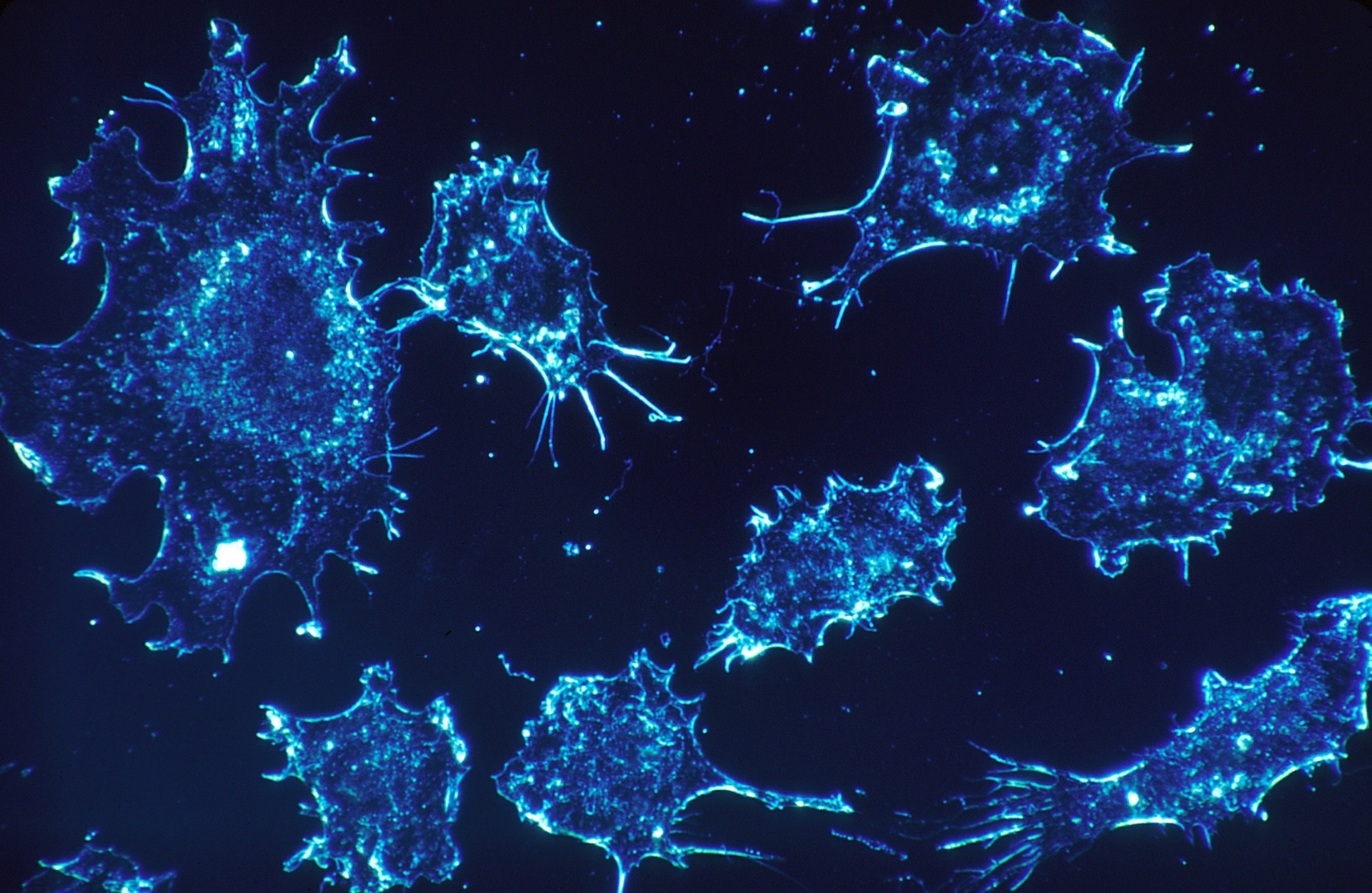
Immunotherapy and cancer
Immunotherapies are also used to help the immune system combat cancer cells in the body. There are several broad types of cancer immunotherapies, but all seek to retrain or boost the body’s response to cancer cells, which often go undetected by the immune system. This summer, James Allison and Tasuku Honjo won the 2018 Nobel Prize in Physiology or Medicine for their innovative work in developing immunotherapy treatments to fight cancer.
“Allison’s and Honjo’s discoveries have added a new pillar in cancer therapy. It represents a completely new principle, because unlike previous strategies, it is not based on targeting the cancer cells, but rather the brakes — the checkpoints — of the host immune system,” Klas Kärre, a member of the Nobel Committee and an immunologist at the Karolinska Institute in Stockholm, said in a statement. “The seminal discoveries by the two laureates constitutes a paradigmatic shift and a landmark in the fight against cancer.”