This tiny wireless device attaches directly to your bones to monitor health

- Engineers at the University of Arizona have developed an ultra-thin wireless computer that attaches directly to the surface of bone.
- The device is able to permanently attach itself to bones, where it can provide doctors with measurements related to bone health.
- The device could also potentially be used to stimulate bone growth by delivering light to bones.
Humans have been breaking bones for a long time. Strategies for managing broken bones were among our earliest surgical techniques, with the earliest examples of bone-fracture surgical appliances dating back 5,000 years to Egypt; in the early 1900s archaeologists discovered two bodies (one with a broken femur and the other with a broken arm) with splints positioned over fractured bones in an ancient tomb at Naga ed-Deir, near Abydos, Egypt.
We are still breaking a lot of bones 5,000 years later. Scientists estimate there are almost 180 million new bone fractures each year, with the most common form of treatment being a plaster cast or metal rod. Basically, we’re still using splints — albeit sophisticated ones.
Although the general strategy for managing a broken bone hasn’t fundamentally changed in 5,000 years, advances in bone health are occurring. However, bone remains a challenging structure to study. As life expectancy increases and bone-related medical problems become more common, the need for new methods of studying and protecting bone health is more critical than ever.
To help meet that need, a team of engineers and physicians at the University of Arizona has developed an ultra-thin wireless computer that attaches directly to the surface of bone. Such devices may someday provide doctors with a new way to accurately monitor bone health in patients, while also potentially opening up new and safer techniques for stimulating bone growth.
Why is bone difficult to study?
Many preliminary studies in biology start in a petri dish, rather than in a living organism. While these artificial environments aren’t perfect, they are close enough for scientists to quickly test early hypotheses before jumping into animal models. However, bone is unique in that it needs mechanical forces (such as the impact of your foot hitting the ground or your bicep flexing) to maintain itself. Combine this with bone’s dense, intricate structure, and you have an environment that is notoriously difficult to artificially simulate. As a result, many bone studies are conducted in living organisms. But how do you study bone if it is buried beneath skin, muscle, and fat?
It isn’t very practical to cut through the surrounding tissue every time you want to run a test on bones. The authors behind the recent study, published in Nature Communications, took a different and more humane approach: implanting a device on the surface of the bone that can run the tests for you. This still requires cutting through the surrounding tissue, but only once. Still, designing a computer that can live on the surface of a bone comes with some challenges.
Positioning, permanence, and power
As you move, your muscles slide across your bones. There is very little space between these two tissues. So, the researchers designed the device to be as thin as a piece of paper (with a length and width roughly the size of the first knuckle on your index finger). This ensured that the device was thin enough to avoid irritating surrounding tissue or become dislodged during muscle movement and also be flexible enough to contort to the bone.
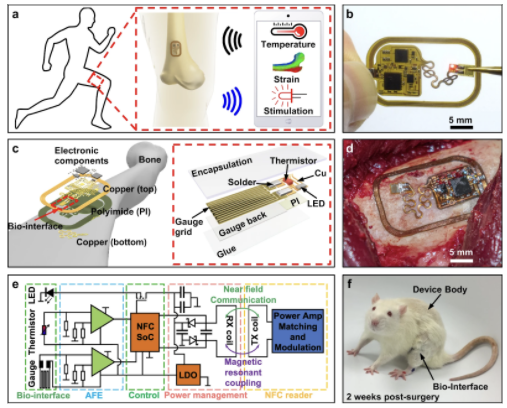
Muscle movement isn’t the only factor that could cause the device to become dislodged. Bone is in a constant state of remodeling, with some cells destroying old bone tissue, while other cells are creating new bone tissue. Due to this, traditional attachment methods would gradually lose adhesion. To address this, study co-author and biomedical engineer John Szivek developed an adhesive that contains calcium particles similar to bone.
With this design, the device is able to form a permanent bond to the bone and take measurements. This opens the doors for studying bone diseases that develop over years, such as Paget’s diseases, which results in fragile, misshapen bones. But how can the device stay powered for years or even decades?
The tiny device does not have a long-lasting battery. In fact, it has no battery at all. The author ditched it to keep the size down. Instead, the team utilized the same technology used in smartphones for contactless payments: near-field communication (NFC), which solved their power problem and also allowed them to communicate with the device.
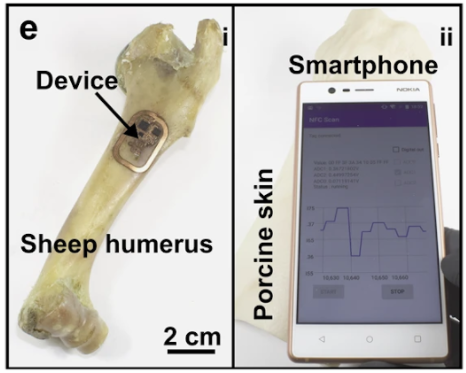
Designing a device that can live on the bone for extended periods with the capacity for wireless power and communication is an impressive feat of engineering. But how does it make it easier to study and protect bone health? The device is also equipped with components capable of measuring bone strength and healing and stimulating bone growth.
Measuring bone strength and healing
To determine whether the device could be used to study how bones are strengthened, the researchers added a strain gauge to measure deformation of the bone. When forces are applied to bone, the bone can compress, expand, twist, and bend. According to Wolff’s Law, a healthy bone will remodel itself to adapt to the force. For example, as a runner’s foot hits the ground, the shin bones compress. For a new runner, the shin bones will compress more than a seasoned runner’s. The new runner experiences more shin strain than the seasoned runner, but, eventually, their bones will remodel to become stronger and resist the compression.
However, if the new runner doesn’t give their shins time to recover, they will develop fractures. It is still unclear what magnitude and duration of force is most beneficial for strengthening bones without risking fractures. It likely varies from person to person. When using strain to strengthen bone, it is important to determine if the bone has healed before applying more strain.
So, the researchers wanted to determine if the device could monitor bone healing. Healthy bone hovers around normal body temperature. But while healing, bone temperature increases as cells work to repair the tissue and more blood flows to the fracture to deliver nutrients. Scientists have shown that monitoring bone temperature has potential for diagnosing the stage in the healing process. Sustained periods of high temperature could suggest complications in the healing. Similarly, if a fracture site has a premature decrease in temperature, it could indicate a sign of interruption of the healing process.
However, this methodology has remained underutilized due to the difficulties of detecting heat through the layers of skin, fat, and muscles. So, the researchers attached a thermistor to measure temperature at the site of implantation. Being able to measure the temperature on the bone itself provides more precise analysis of the healing process.
Finding the goldilocks zone of strain magnitude and healing duration would improve therapies toward treating osteoporosis, which affects an estimated 200 million people worldwide. Osteoporosis does not just affect the aged. It is also a common problem for individuals with physical disabilities: children with cerebral palsy, for example. However, given our lack of understanding of how bones are strengthened (especially at young ages), children’s fragile bones are treated through pharmaceuticals, which can cause problems with bone growth during adulthood.
Stimulating bone growth
Strain is not the only method of stimulating bone growth. Recent studies have shown that light can be used to stimulate bone regeneration. However, to reach the bone, the high energy light must penetrate layers of other tissues, which can damage those tissues. The authors sought to determine whether their device was capable of delivering light stimulation, while simultaneously collecting data. A light source directly on the bone would mean lower energy light sources could be utilized, reducing the risk of collateral damage.
Imagine you fracture your femur and your physician implants this device to stimulate healing and monitor the temperature. When the temperature starts to get too high, light stimulation could be reduced. And since the device utilizes the same NFC common to cell phones, individuals could monitor and intervene without visiting a physician.
“This offers unprecedented opportunities for mechanistic studies of osteogenesis and pathogenesis of musculoskeletal diseases, as well as the development of new types of diagnostics and therapeutics,“ the authors wrote.